Top 5 things RVTs Should Know About Rabies Testing in Ontario
World Rabies Day (WRD) is observed annually on Sept 28th to raise awareness about rabies on the anniversary of the death of Louis Pasteur who discovered the first rabies vaccine in 1885.
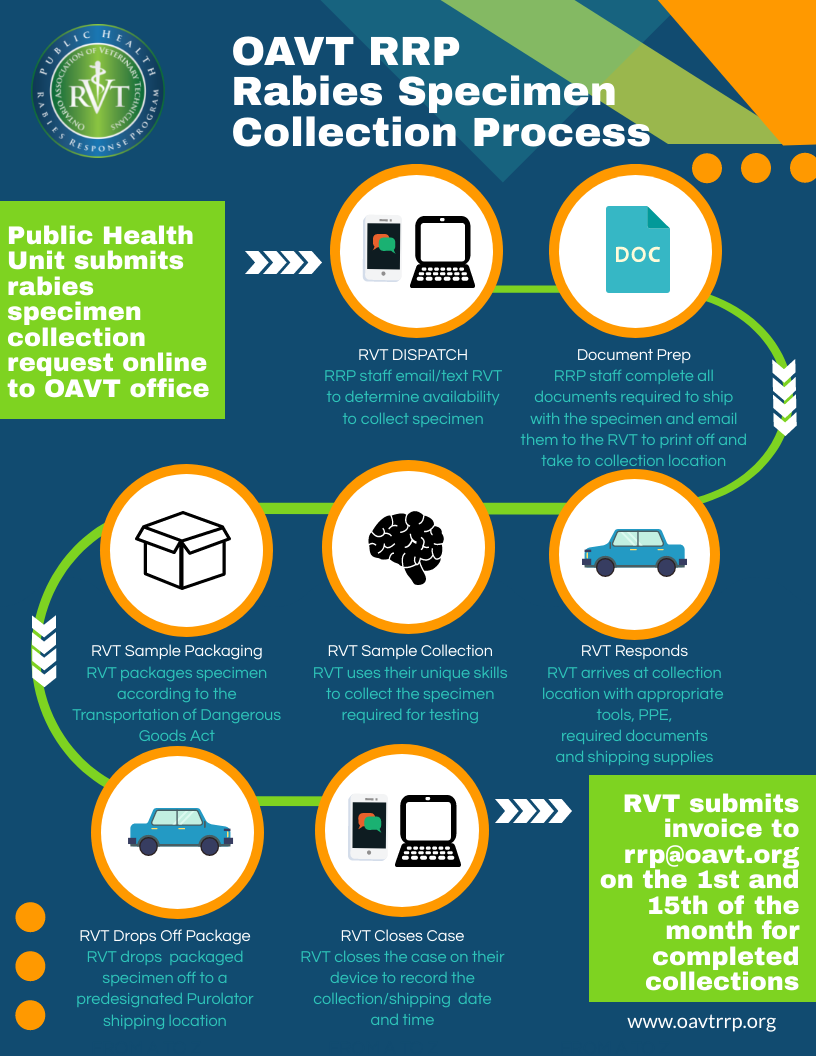
Since 2015 the OAVT Public Health Rabies Response Program has trained RVTs to collect and ship 10,000+ rabies specimens for rabies testing/surveillance in Ontario at the request of the Ministry of Health and Ontario Public Health Units when a human has been exposed to an animal potentially carrying rabies. Many of these specimens are collected from veterinary hospitals, animal shelters and wildlife rehabilitators.
Here are the top 5 things RVTs should know about testing animals for rabies in Ontario.
1. Who to call when you need to report a rabies exposure or Sick Wildlife
In Ontario rabies surveillance is provided through three different provincial Ministries:
- The Ministry of Health (MOH)/local Public Health Units (PHUs) are responsible for animal-to-human exposures.
- The Ministry of Agriculture, Food and Agribusiness (OMAFA) is responsible for animal-to-animal exposures.
- The Ministry of Natural Resources (MNR) is responsible for terrestrial wildlife with no human or animal exposure displaying signs of rabies.
Check out the Rabies Suspect Animals Who To Call When for a breakdown on who to contact to report a potential rabies exposure or sick wildlife.
2. When to report a potential rabies exposure or sick wildlife
In Canada, rabies is a federally reportable disease under the Health of Animals Act, and all suspect cases must be reported to the Canadian Food Inspection Agency (CFIA). This can be done by contacting a CFIA district veterinarian. There are also provincial requirements to report rabies in Ontario.
Animal to Human Exposures
Rabies is also covered under Regulation 557: Communicable Diseases – General of Ontario’s Health Protection and Promotion Act where it states that:
2. (1) A physician, registered nurse in the extended class, veterinarian, police officer or any other person who has information concerning either or both of the following shall, as soon as possible, notify the medical officer of health and provide the medical officer of health with the information, including the name and contact information of the exposed person:
1. Any bite from a mammal.
2. Any contact with a mammal that is conducive to the potential transmission of rabies to persons.
(2) The owner or the person having the care and custody of an animal,
(a) that has bitten or is suspected of having bitten a person; or
(b) that is suspected by the medical officer of health of having rabies,
shall provide the medical officer of health with such information and assistance with respect to the animal as the medical officer of health requires.
The Ministry of Health’s document The Management of Potential Rabies Exposures Guidelines 2020 indicates that “Rabies is transmitted only when the virus is introduced into a bite wound, open cuts in skin, or onto mucous membranes such as the mouth or eyes.” This most often occurs with the introduction of saliva from an infected animal but can also include exposure to neural tissues. The document also states that “The ministry’s Public Health Veterinarian should be notified of any animal suspected of being rabid on the basis of a veterinary examination, regardless of whether it has been involved in a biting incident”.
Note: the rabies vaccination status of an animal or person does not preclude the exposure from being reported.
Animal to Animal Exposures
Under section 5.2 of Canada’s Health of Animals Act veterinarians should also report exposures to domestic animals from other domestic animals or wildlife in certain situations. The Ontario Ministry of Agriculture, Food and Agribusiness outlines these instances here.
Sick Wildlife with No Human or Animal Exposure
If a wild terrestrial animal is suspicious of having rabies and has had no human or animal contact the animal should be reported to the Ministry of Natural Resources. They are legislated under Ontario’s Fish & Wildlife Conservation Act to establish a wildlife disease control and surveillance zone if the Minister is of the opinion that,
(a) the wildlife disease may have serious adverse impacts on wildlife populations or serious adverse ecological, social or economic impacts in Ontario; and
(b) the order may assist in controlling or eradicating the wildlife disease, minimizing its impacts in Ontario or reducing the risk of the wildlife disease entering Ontario.
3. How to position and prepare animals requiring testing
If you are reporting an incident involving an animal bite or scratch, or potentially infected saliva or neural tissue contact to an open wound or mucous membrane, to your local Public Health Unit and the animal is already deceased there is a possibility that rabies testing will be required. How you store the animal prior to specimen collection is important for the quick collection of required tissues for testing.

This positioning allows the RRP RVT easier access to disarticulate the head when there is not time to thaw the animal prior to their arrival. Find the RRP info sheet here outlining these tips.
4. What labs provide rabies testing in Ontario?
The following laboratories provide rabies testing in Ontario:
- Canadian Food Inspection Agency (CFIA) most often performs Fluorescent Antibody Testing (FAT); the gold standard rabies test worldwide. They also provide rabies variant typing.
- Ministry of Natural Resources (MNR) performs Direct Rapid Immunohistochemical testing (dRIT); a field test commonly used in wildlife. Positive results are sent to the CFIA for confirmatory FAT.
- Canadian Wildlife Health Cooperative (CWHC) performs Direct Rapid Immunohistochemical testing (dRIT); a field test commonly used in wildlife. Positive results are sent to the CFIA for confirmatory FAT.
5. How to obtain results
Animal To Human Exposure Results
If an animal in your care has been tested for rabies, at the request of your local public health unit, results will be returned directly from the CFIA to the Public Health Unit who ordered the testing. The CFIA can take up to 72 hours to produce results from the time the specimen arrives at the CFIA lab. In most cases results are released the same day the specimen is received by the lab. For a copy of the results please reach out to the Public Health Inspector who is assigned to the case. If you are unsure of who the inspector is you can find the general contact information for your local PHU here .
Animal to Animal Exposure Results
If an animal in the care of your hospital or shelter has been tested for rabies in consultation with and at the request of OMAFA, a copy of the results will be sent to you from the CFIA directly and OMAFA will also follow up by phone to relay the results.
Sick Wildlife with No Human or Animal Exposure Results
If you have reported a sick wild terrestrial animal to MNR and they have have proceeded with testing you can follow up for the test results by contacting their rabies information line 1-888-574-6656 or by email at rabies@ontario.ca.
If the animal was tested through your local Public Health Unit the results are returned directly from the CWHC to the Public Health Unit who ordered the testing. The CWHC can take up to 4-6 weeks to produce results from the time the specimen arrives at the CWHC lab. For a copy of the results please reach out to the Public Health Inspector who is assigned to the case. If you are unsure of who the inspector is you can find the general contact information for your local PHU here .
Looking for information about rabies?
For information about rabies visit the OAVT RRP Rabies Resources page and the OAVT RRP Rabies Public Portal.
In this section
RRP Info Sheets For Veterinary Hospitals & Animal Shelters
All veterinary staff can help with the efficiency and accuracy of the OAVT RRP. Here are some tips for:
- Preparing For A Specimen Collection-Small Animal Hospital Teams
- Preparing For A Specimen Collection- Large Animal Hospital Teams
- Preparing For A Specimen Collection- Animal Shelter Teams
- Specimen Positioning & Storage Prior to Collection
- Bat Euthanasia Information Sheet
- RRP Post Collection Info For Veterinary Hospitals/Shelters
- Who to Call When For Rabies Testing?
- Top 5 Things RVTs Should Know About Rabies Testing in Ontario
How do I become an RVT
Whether you are an Ontario student or internationally trained graduate, learn about the five steps it takes to become a Registered Veterinary Technician.
Job Board
Search through Ontario’s #1 source for animal healthcare jobs. New jobs are posted daily.
RVT Registry
The official Registry of Ontario’s Registered Veterinary Technicians. All RVTs in good standing can be found in this searchable Registry.